
PCs say mandatory naloxone program for high-risk workplaces first of its kind in North America
The PC government is making it mandatory for certain “high risk” workplaces to have naloxone kits on site in the event of an opioid overdose.
Naloxone (also known under the brand name Narcan) can temporarily reduce the effects of an opioid overdose. When someone consumes too much of an opioid, the drug begins to interrupt critical processes within the body, including the natural instinct to breathe. If administered in time, naloxone can significantly increase the chance of survival by opening up the airways, giving paramedics or other trained medical professionals the chance to intervene. These extra few minutes (on average) can drastically reduce the number of fatal overdoses.
The new program has been billed as a preventionary measure in workplaces that run the higher risk of seeing opioid-related overdoses. According to the Ministry of Labour, Immigration, Training and Skills Development, it was created “following extensive stakeholder consultations, including a Regulatory Registry posting that was open for public comment.”
While the increased presence of naloxone in workplaces across the province will help in the event of an emergency, it remains unclear how many employers will actually be legislated to carry naloxone under the requirements of the new program.
Amendments to the Occupational Health and Safety Act (OSHA), as of June 1, dictate that any workplace where an overdose may have occurred; or there is a risk of a worker overdosing on the job are required to have naloxone on site. The Act defines the “risk of an opioid overdose” as any workplace that meets any of the following criteria:
-
An opioid overdose may have already occurred in the workplace.
-
A worker who uses opioids may voluntarily disclose this risk to their employer.
-
An employer may observe opioid use among workers in their workplace or discover that opioid use is occurring in their workplace during a workplace investigation.
-
An employer may find discarded opioid paraphernalia, such as used needles, in their workplace.
-
The joint health and safety committee (JHSC), health and safety representative (HSR), a union representative, human resources (HR) staff, and/or someone else in the workplace may bring this risk to the employer’s attention.
However, even if one of these requirements are met, it still may not require the employer to provide naloxone. The Ontario website states: "If an employer is aware that one of their workers uses opioids as prescribed by a medical practitioner, it is unlikely that this would, alone, create an awareness of the potential risk of a workplace opioid overdose because such use is under medical supervision,” the website states. “If the employer is not or has not become aware of a risk of one of their workers having an opioid overdose at the workplace, an employer would not need to comply with the OHSA requirements to provide naloxone in the workplace.”
If a workplace meets the criteria to be classified as high risk, a free naloxone kit will be provided by the Province along with free training for two workers.
According to a PC press release, construction and manufacturing employers account for 45 percent of participating workplaces. Others include retail (9 percent); healthcare and social assistance (9 percent); accommodation and food service (7 percent); arts, entertainment and recreation (4 percent), and 25 percent are classified as “other”.
Close to one third of employed drug poisoning victims worked in the construction industry, according to government data. Studies have found a variety of factors driving those in the sector to seek out non-prescription opioids.
“Importantly, despite a high prevalence of pain among workers, prescription opioids are not driving the patterns seen in this industry, with most deaths involving a combination of opioids with other drugs and alcohol. This could reflect a reliance on non-prescription opioids to manage unresolved pain in a sector where workplace culture and lack of job security can lead to under-reporting of injuries and pressure to minimize recovery time,” Dr. Tara Gomes, a lead author of a report by researchers from the Ontario Drug Policy Research Network (ODPRN), and scientist at the Li Ka Shing Knowledge Institute of St. Michael’s Hospital and Institute for Clinical Evaluative Sciences states.
The PCs say the program is the first of its kind in North America, but similar prevention programs can be found in other jurisdictions. In 2018, Kingston City Council voted to stock the medication at 14 public venues including museums, parks, and at city hall. New York state officially enacted legislation in October 2022 mandating naloxone be stocked in all bars across the city, and the Department of Labor awarded grants from 2019-2022 to workplaces for things like prevention training.
According to a representative for MPP Monte McNaughton, Minister of Labour, Immigration, Training, and Skills Development, even if a business is not eligible for a free kit and training under the Workplace Naloxone Program, they may independently choose to keep a naloxone kit on hand and provide training to their employees.
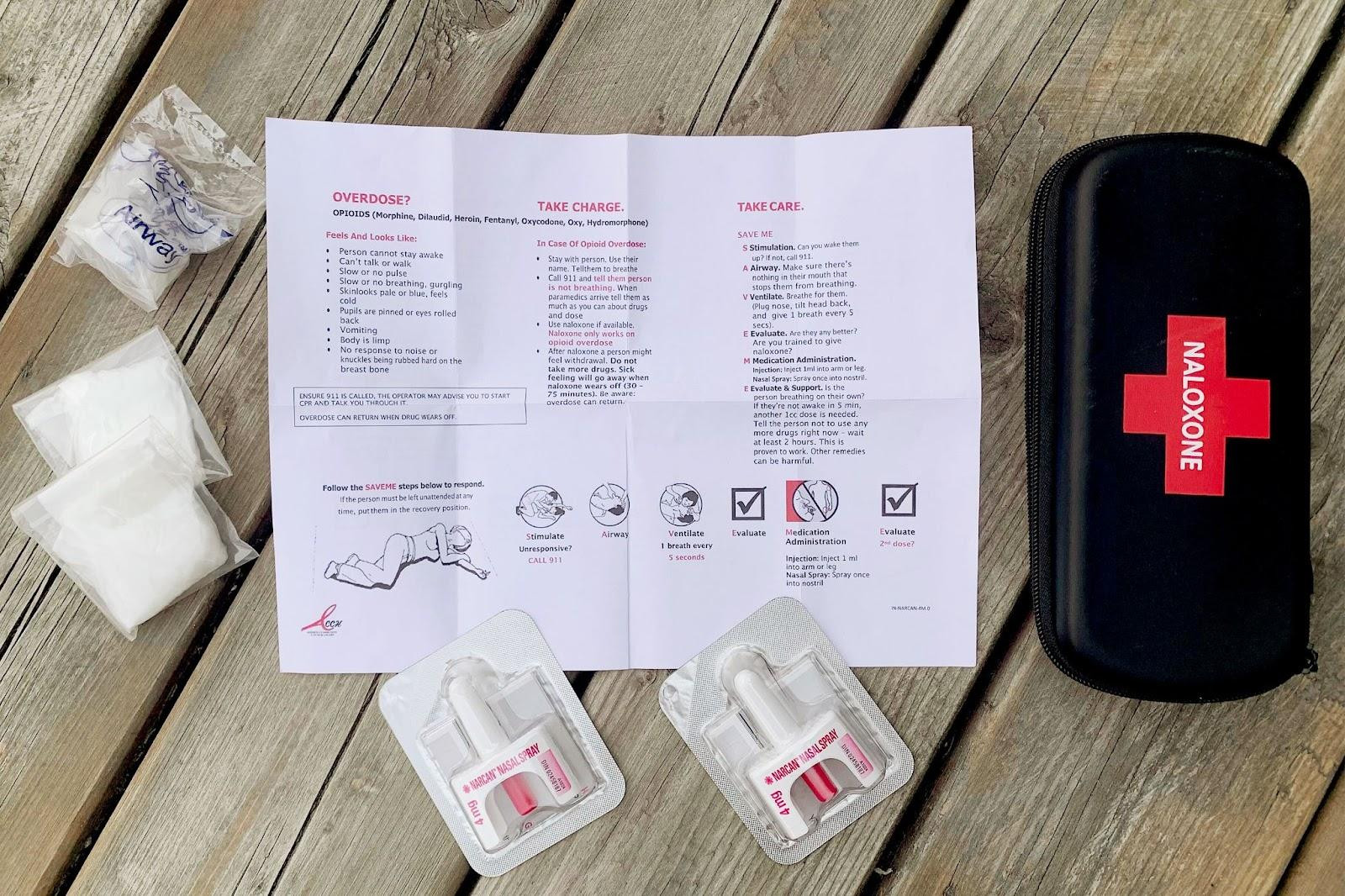
Participating pharmacies across Ontario carry free Naloxone (Narcan) kits including two nasal sprays with four doses each.
(Alexis Wright/The Pointer)
Overdoses due to opioids have been particularly concerning due to the sharp increase in contaminated substances within the street drug supply. Among the most common contaminants is the synthetic opiate Fentanyl—1,000 times stronger than morphine.
“Anyone who is not obtaining their substances from the pharmacy or uses opioids, regardless of their source, is at risk,” says Alison Watson, a nurse practitioner with the Centre for Addiction and Mental Health (CAMH), noting that even taking opiate medications as prescribed by professionals comes with risks.
Analogs, drugs similar in chemical structure to fentanyl but not routinely detected because specialized toxicology testing is required, are even riskier. The most common being acetylfentanyl, furanylfentanyl, and the strongest, carfentanil—originally manufactured to tranquilize large animals like elephants and is 10,000 times more potent than morphine. Because these synthetic opioids are odorless, white powders, it is common to be laced with other drugs like stimulants such as cocaine or methamphetamine. In the Region of Peel between 2020 and 2021, 90 percent of opioid related deaths involved fentanyl.
“We are encouraged by the Ministry of Labour, Training, and Skills Development’s efforts in recognizing the important roles employers and workplaces could play responding to the ongoing drug poisoning crisis which has worsened during the COVID-19 pandemic,” the Canadian Mental Health Association (CMHA) said in a statement in January 2022 when the proposed legislation was open for consultation.
Since then nearly 10 Ontarians have died per day due to opioid poisoning leading to overdose, almost all of them accidental.
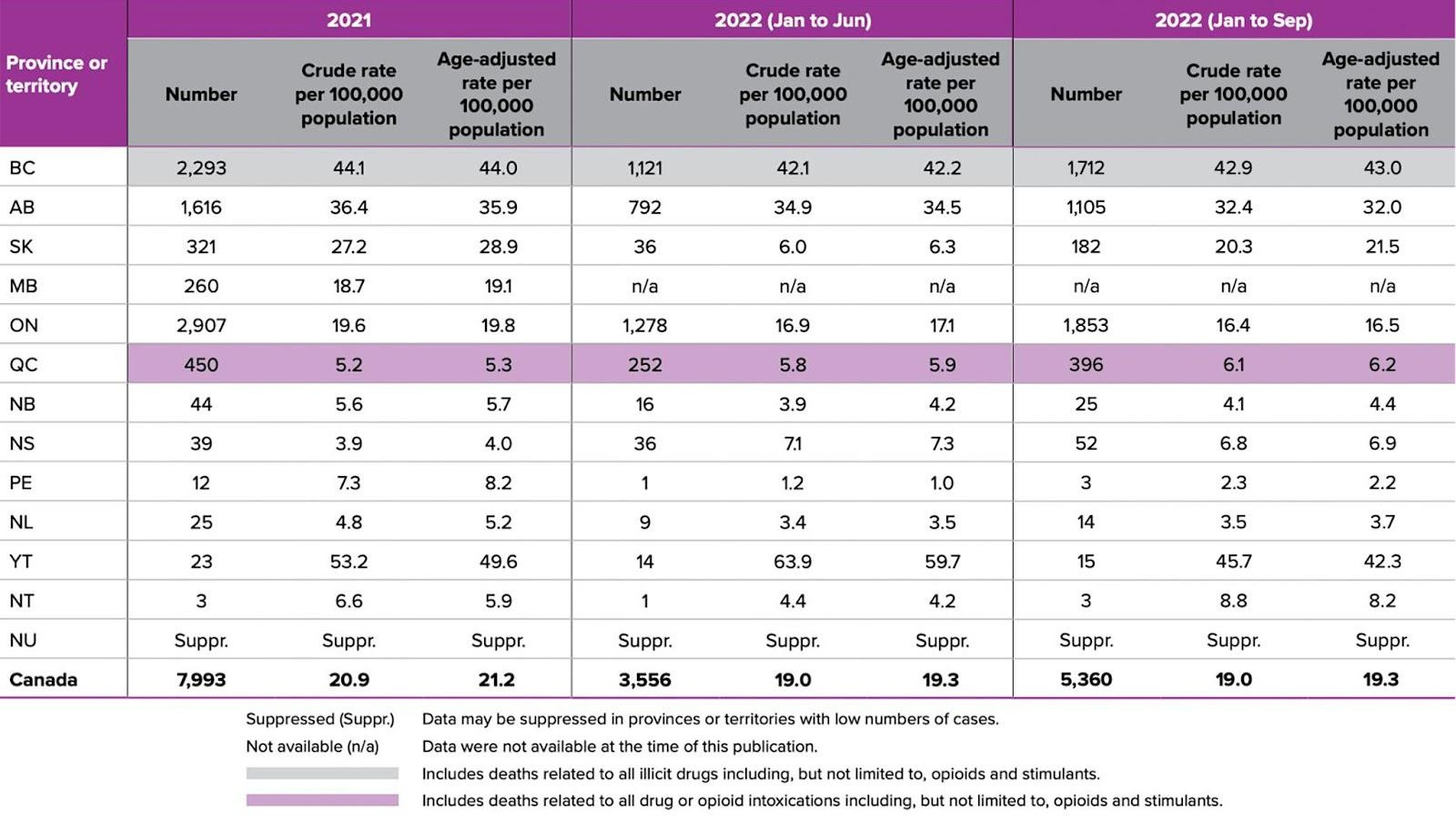
In 2016, Canada saw over 2,800 deaths due to opioid toxicity and in 2021, nearly 8,000 people died, showing the extreme rise in overdose during the COVID-19 pandemic.
(Health Canada)
Health experts have been calling for naloxone to be provided in the workplace for years as the opioid crisis has continued to grow despite the efforts of organizations on the ground to help those in need.
Between January and September 2022, there have been 1,853 opioid related deaths in Ontario. In Peel, overdose deaths increased sharply in 2017 rising from 3.1 deaths per 100,000 the previous year to 5.4 per 100,000, and continued upward. Between 2017 and 2021 opioid-related deaths in Peel rose 133 percent—the majority among the region’s younger population. According to Peel Public Health the deaths were most common among adults aged 25 to 44 years
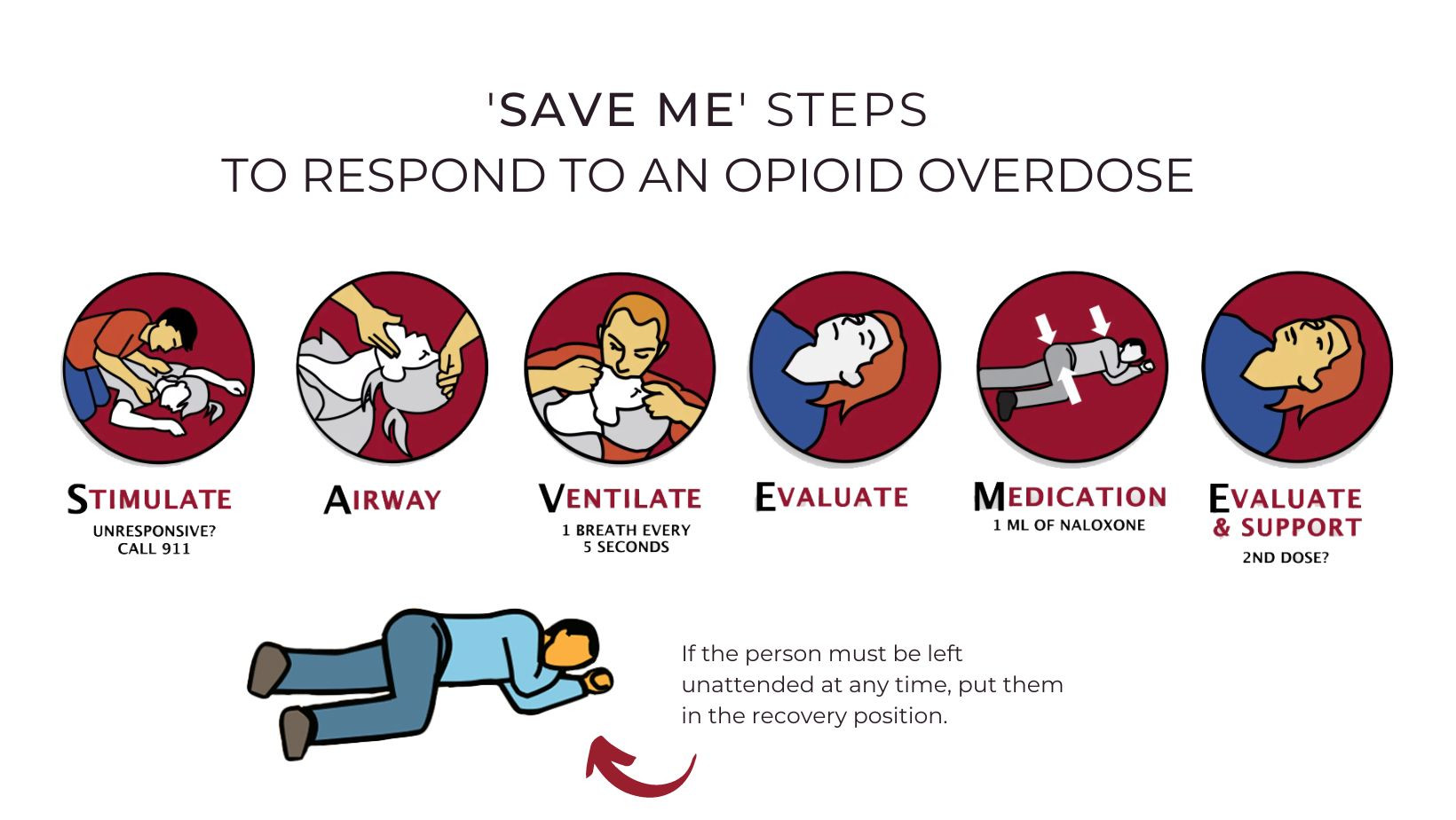
Included in Naloxone kits available to the general public are information pamphlets that detail the steps under the easy to remember acronym ‘SAVE ME’ on how to effectively respond to an opioid overdose.
(Alexis Wright/The Pointer)
Part of the stigma surrounding overdose contributes to how institutions respond to the crisis. Medical kits and AEDs (Automated External Defibrillators) are required by law on all public premises. The idea to stock naloxone along with other legislated life saving measures was first brought into public discussion over five years ago.
Minister McMaughton has previously stated he hopes to expand the program to include every place of employment in the province by 2030, but a plan to do so has yet to be shared.
If required in all workplaces, high-risk or not, there is a higher chance of more people, including those who unknowingly ingest opioids—a scenario becoming more common—receiving life-saving medication and giving medical professionals more time to respond, ultimately lowering the overall chance of accidental death.
Email: [email protected]
Twitter: @lextoinfinity
At a time when vital public information is needed by everyone, The Pointer has taken down our paywall on all stories relating to the pandemic and those of public interest to ensure every resident of Brampton and Mississauga has access to the facts. For those who are able, we encourage you to consider a subscription. This will help us report on important public interest issues the community needs to know about now more than ever. You can register for a 30-day free trial HERE. Thereafter, The Pointer will charge $10 a month and you can cancel any time right on the website. Thank you
Submit a correction about this story


