
‘Nothing has changed’: Province ignores mental health and addictions crisis in Peel, children waiting up to 737 days for help
Thousands of children and youth in Peel are experiencing mental health crises every year, and they’re dealing with it on their own.
A chronically underfunded public health system that has not kept up with the fast-paced growth in the region, a dramatic rise in mental health issues and a provincial government that appears unwilling to properly address the crisis, has left those under the age of 18 languishing on waitlists for more than two years to get life-saving help.
The scope of the problem has worsened during the COVID-19 pandemic.
On Thursday, David Smith Chief Executive Officer of the Canadian Mental Health Association (CMHA) Peel Dufferin, an advocate for reforming the funding of mental health support in Peel, appeared before regional councillors. He asked them again for help to pressure Queen’s Park, which has ignored the growing crisis in the region.
Smith’s organization is one of the lowest funded branches of the CMHA in Ontario, receiving about a third of what other areas receive per capita, which prevents it from reaching about 90 percent of the people who need help in Peel. That was before COVID-19 forced people to stay indoors and led to sky-rocketing anxiety and mental health concerns among the Canadian population.

David Smith, CEO of CMHA Peel-Dufferin
Smith says CMHA Peel Dufferin has seen the number of people seeking its services rise 40 percent during the pandemic and a 30 percent spike in crisis calls has been recorded over the last three months. These emergency calls include people contemplating self-harm or suicide.
The issue is not isolated to Peel, as data from Statistics Canada from early in the pandemic shows people across the country are dealing with increased anxiety as a result of the challenges the novel coronavirus has presented. Prior to COVID-19, approximately 1 in 5 people in Canada experienced a mental health problem or illness in a given year, this represents about 300,000 people in Peel.
In Peel, though, those on the front lines of this mental health crisis are fighting with one hand tied behind their back.
The Central West LHIN, which includes Brampton, and the Mississauga Halton LHIN, received $66 and $53 respectively per capita from the provincial government for mental health and addictions support, well below the provincial average of $107 per capita. Much of this funding is targeted to specific agencies, which helps the individual agency and its programming, but can create siloed efforts in the community that are not interconnected, making it difficult for those in need to access them.
The situation gets even worse when drilling down to those who are in desperate need. For people in crisis or suffering serious withdrawal due to their addiction, Brampton and Mississauga have few resources available to help.
The Mississauga Halton LHIN currently has one mental health bed per 78,500 people, while Brampton and the Central West LHIN have one per 66,808 people. By comparison, in Toronto Centre, one of the top-funded areas for these sectors, there is one mental health bed for every 3,500 people, meaning the two cities have about 5 percent of the mental health capacity compared to central Toronto, an area that does see high levels of homelessness and mental health crisis.
Mississauga and Brampton also make do with about 7 percent of the psychiatric resources compared to other parts of the province, leaving those looking to get help for their mental health or addiction problems from a professional, with very few places to turn.
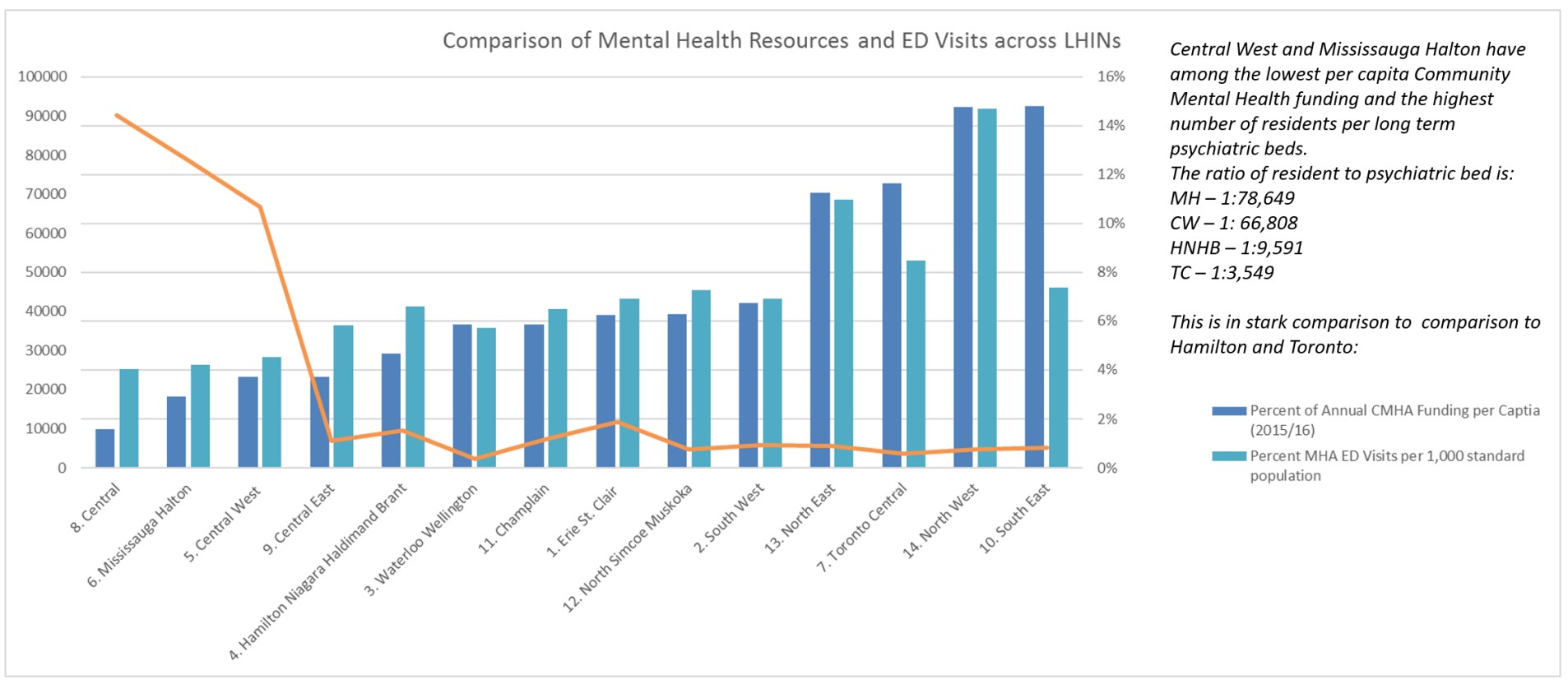
The chart above highlights the Central West LHIN (which includes Brampton) and the Mississauga Halton LHIN, at the far left, the two lowest funded regions in the province.
For children and youth mental health services, Peel receives approximately $22.3 million annually, three times less than the provincial average of about $66 million and about six times less than the $133 million received by Toronto. This is particularly worrisome in a young region, where 70 percent of mental health problems have their onset in childhood or early adolescence, according to the Centre for Addiction and Mental Health.
Peel Region is home to 12 percent of the province’s children under the age of 19, with a fast growing population that is projected to continue increasing rapidly over the next two decades. There are currently 550 children/youth that are waiting for counselling services.
Brampton and Regional Councillor Rowena Santos (Wards 1 & 5) has spoken with teachers and principals at schools and was shocked by their stories.
“All of the staff have expressed significant concern over children as young as kindergarten age to high school about being suicidal or doing self-harm,” she said.
The utter lack of available services leaves those in Peel, including young children, throwing their hands up, and turning away from the system out of frustration.
“Most people just give up, and stay at home and suffer in silence and get some minimal treatment and carry on,” Smith said.
Those who are unable to get help then turn to other ways of coping with mental illness, which can include drugs and alcohol, or self-harm, further exacerbating their issues and eventually placing further pressure on the system as their illness worsens and requires more complex care.
Many councillors around the regional table were not shocked by the numbers. They have seen them all before.
Mississauga Councillor Pat Saito said she remembers waitlists for psychological services in the Mississauga area stretching out between 6 months to a year – 25 years ago.
It’s the same story in Peel’s addictions sector where CMHA Peel Dufferin is also a key player on the front line of the opioid crisis.
Since 2006, Peel has evolved into one of the deadliest regions for fentanyl-related deaths in Ontario, with Peel Public Health recording 58 overdoses involving the drug in 2017, behind only Waterloo, with 67 deaths, and Toronto, with 218. The Simcoe Muskoka District Health Unit also recorded 58 overdoses involving fentanyl that year.
Since 2003, deaths caused by opioids overall have risen by 246 per cent. In 2017, more than 1,250 Ontarians died from opioid-related causes.
In Peel, between 2005 and 2013, the number of opioid-related deaths has remained steady, averaging about 26 per year. There were spikes in 2014, which saw 45 deaths, and in 2017, with 81 deaths.
“The province continues to nod its head and recognize that it’s an issue but nothing has changed,” said Ward 3 Mississauga Councillor Chris Fonseca during Thursday’s meeting.
“There seems to be the same grind,” said Brampton Councillor Martin Medeiros, adding that the stories detailing the crisis and the apathetic response feels like groundhog day.

Brampton and Regional Councillor Martin Medeiros
If councillors are feeling a sense of deja vu, it’s because mental health and addictions is not the only sector that is underfunded in the region. Services for sexual assault survivors, healthcare in general and court services, to name a few, all receive some of the lowest levels of investment anywhere in the province.
The entire public health system in Peel, which includes the mental health and addictions programming offered by the region, has been chronically underfunded for decades
The majority of Ontario’s 35 health units have relied on the provincial government for about 75 percent of their funding, while local municipalities made up the remaining 25 percent. Under new plans announced by Health Minister Christine Elliott last year, municipalities will now be responsible for 30 percent of their public health budgets.
This would be nothing new in Peel Region, where the provincial contribution has typically only accounted for 63 percent of the Peel Public Health budget, with the regional municipalities making up the remaining 37 percent.
The most recent numbers from the province show an increase in funding for Peel Public Health this year. In total, Peel is getting just over $58 million for public health programs, up from its 2018 allocation of $54.1 million. The region is also receiving a one-time grant of almost $30,000 for a needle exchange program.
These numbers are far from the full picture, as Peel has been underfunded for years compared to many other parts of the province, forcing Public Health to take on new challenges such as increased mental health risks, the opioid crisis and the rising impact of deadlier drugs like fentanyl, with effectively the same budget.
In terms of underfunding, Councillor Saito said "COVID is just making it worse. It's escalating the problem."
In March, Premier Doug Ford announced a new provincial mental health strategy and promised to spend $1.9 billion on mental health related initiatives over the next decade. Scheduled to launch this spring, the province has said the plan will include $20 million in new funding this year for mental health and addiction programming. No further details have been released to date and it’s unclear how much Peel will get.
While this may be “new” funding, municipalities are also grappling with the new financial realities created by COVID-19, which has blown a hole in many city budgets, and it remains unclear if the provincial cuts to healthcare and public health sectors, initially put off this year, will still go ahead in 2021 as planned.
The new funding announced recently doesn’t help organizations like those in Peel that have been drastically underfunded for years. Smith explained that, typically, funding is based on the amount an organization received the year before, with a minimal increase. This generally works in areas where the population is steady, but has a disadvantage for areas with fast growing populations like Peel’s.

Mississauga and Regional Councillor Pat Saito says not much has changed in 25 years
In April 2019, the provincial budget introduced sweeping cuts to public health units across the province. The move drew strong backlash, prompting damage-control efforts at Queen’s Park. Initially, it was announced that cuts that would have cost the public health units millions of dollars would be retroactive, meaning they would affect the current year’s budget. Following the uproar, the cuts were pushed to 2020. Speaking at the recent Association of Municipalities of Ontario (AMO) conference in Ottawa, prior to the COVID-19 pandemic, Ford said the cuts will move ahead next year.
The Region of Peel has tried previously to get the province’s attention about the lack of funding for key programs in Peel. Following the announcement of the provincial cuts last year, the region launched its #FairShareforPeel campaign to bring more attention to the issue. Similar campaigns have popped up over the last decade, with little success.
“Nobody down there (at Queen’s Park) really cared. It fell on deaf ears,” Councillor Saito said of the latest fair share for Peel campaign.
It’s not clear what other actions have been taken by council or regional staff, aside from sending letters to the province, or trying to start hashtags on social media.
While the region is beholden to the province when it comes to financial assistance to fund the programs to assist those with mental health conditions or those battling addiction, councillors can use their powers to attack many of the root causes of addiction and mental health issues. However, local elected representatives have largely ignored these issues and funding in areas that could greatly alleviate the risks.
During budget season at the Region of Peel, many of the same councillors blaming the province for underfunding, fail to allocate adequate regional resources to social services and other areas, while other budget areas, such as policing, get what leaders in those sectors ask for.
A quick look at the region’s affordable housing budget, for example, which has seen miniscule increases over the last two years, highlights one area in particular that councillors could focus on instead of always pointing fingers at the province. Regional councillors have funded less than 5 percent of what was needed to meet the 2018 to 2028 affordable housing strategy that staff had created, which was approved by council, then ignored by members when it came time to fund the program.
Regional Chair Nando Iannicca referred to the Greek myth of Sisyphus, endlessly pushing his boulder up the hill, only to have it roll back down, as a similar task as trying to get the province to address the underfunding problems in Peel. Yet, it appears councillors are going to try and push that boulder up the hill one more time, with another campaign to get the province’s attention.
Initially, a motion was to be passed Thursday for staff to continue advocating at Queen’s Park for proper, fair share funding. However, after discussions, it was determined that the motion should be sent back to staff for further attention and more “aggressive” language.
Councillor Saito said the region has never had an “MPP champion” at Queen’s Park to tackle this issue. It doesn’t appear that they have one now either. Requests for comment on Peel’s mental health and addictions crisis and efforts to increase funding to the region, sent to Brampton’s two PC MPPs, and Mississauga six PC MPPs, did not receive responses ahead of publication.
Aside from an announcement in May 2019 of a $2.3 million grant for harm-reduction efforts to the Canadian Mental Health Association (CMHA) Peel-Dufferin, it’s not clear what other investments the province has made to assist Peel directly.
Along with mental health services, Peels addiction centres are another growing concern on the list of things that need support.
Meanwhile, the ongoing pandemic is making the crisis even worse.
Email: [email protected]
Twitter: @JoeljWittnebel
Email: [email protected]
Twitter: @taasha__15
COVID-19 is impacting all Canadians. At a time when vital public information is needed by everyone, The Pointer has taken down our paywall on all stories relating to the pandemic to ensure every resident of Brampton and Mississauga has access to the facts. For those who are able, we encourage you to consider a subscription. This will help us report on important public interest issues the community needs to know about now more than ever. You can register for a 30-day free trial HERE. Thereafter, The Pointer will charge $10 a month and you can cancel any time right on the website. Thank you.
Submit a correction about this story


