
Timely, localized data is vital in vanquishing COVID-19
Peel Public Health and the Ontario Ministry of Health release updates on rates of COVID-19 infections on a daily basis. While the regional and provincial governments are transparent on this front, there is no data publicly available on hospital patient statistics and what the picture in specific areas of communities looks like.
If a cluster of outbreaks is occurring in a specific neighbourhood because of a super-spreader (an individual who transmits the virus to a much larger number of people than most who are contagious) public health officials might eventually pick up on the trend, but it's difficult for community members to know what is happening in their own backyard. This is why localized data and getting it out to the public is crucial.
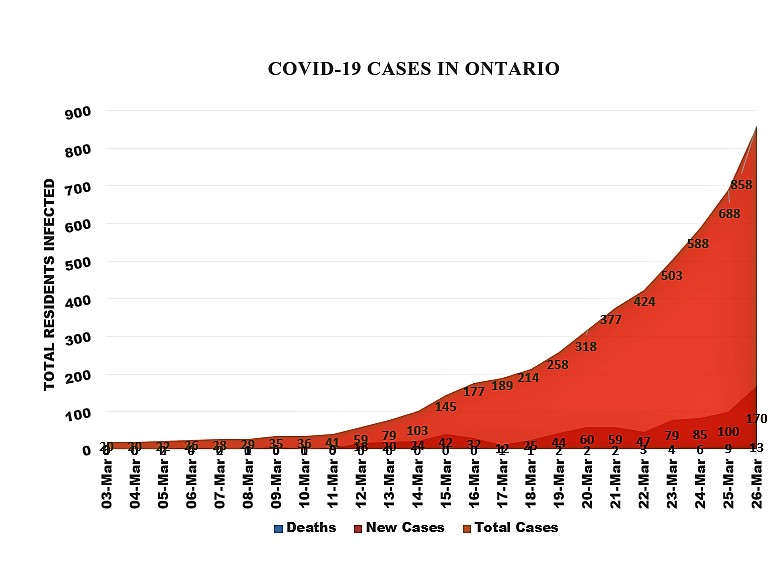
There are 688 cases of the novel coronavirus in Ontario to date. Of these, 319 (46.37 percent) are in Toronto while 75 of the cases (11 percent) are in Peel Region, as of Wednesday. Looking at the local numbers is much more useful than national or even provincial data, which does not account for communities that have high rates and communities that have low rates — they are all just lumped together.
As of Wednesday evening Canada reported 3,385 cases of COVID-19. But if this puts some at ease because the number is much lower than, for example, the U.S. total of 52,000 (according to the World Health Organization) consider this. New York state has about 27,000 of those reported cases. This means the rest of the country has about 25,000 cases. The population of the US, not including New York state, is about 310 million residents. So Toronto has about one percent of the US population not including New York. If you take the Toronto COVID numbers and use a per capita comparison with the US, not including New York state, Canada's largest city has a higher rate of COVID-19 infection, about 1.07 infected people per 10,000 residents, compared to about 0.81 infected individuals per 10,000 in the US, when New York state is not included. But even this is not an accurate comparison considering large segments of the US population have much lower rates than the national per capita figure.
Peel's current rate of infection is about 0.50 per 10,000 residents, compared to the Canadian rate which is about 0.90 per 10,000 residents. Canada's current rate is actually higher than the US rate, when New York state is removed from the equation.
When we consider large portions of the geography of Canada where rates remain very low, it becomes clear that clusters in centres such as the GTA, the Greater Vancouver Area and the Montreal metropolitan area have much higher rates than people might realize and are probably at a greater risk of seeing their rates of infection grow far higher than the overall Canadian rate.
The chart below has been updated since the data used above and reflects Ontario reporting as of Thursday morning
Jeffery Rosenthal, a statistics professor at the University of Toronto, told The Pointer with a situation like the COVID-19 pandemic, the more specific information on the spread of the disease available to the public, the better. “The more we know about that, first of all, the more we can try to take steps with things like social distancing and disinfecting and all these things to try to reduce the spread of it in those spaces targeted. And also, people can be warned and we can plan for medical cases that might be coming in,” Rosenthal said.
It’s no secret that government communications teams are doing their best to answer the barrage of requests for information about the rapidly changing circumstances of the COVID-19 pandemic. However, when general statements lack specific information, there’s a disconnect with the public on the current situation.
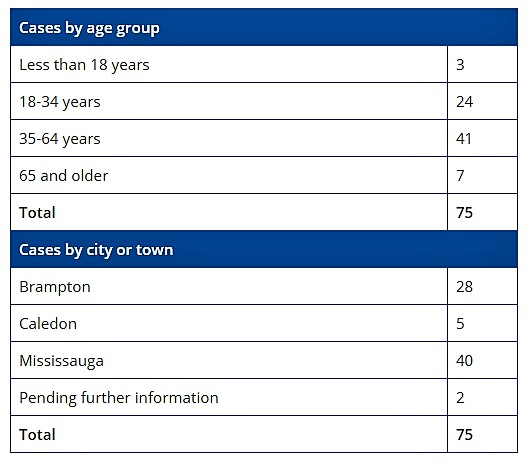
Data from the Region of Peel as of Thursday morning
The lack of specific COVID-19 information available to Peel is a massive issue for a region with struggling healthcare systems. In January, the City of Brampton declared a healthcare emergency, asking the province for help to end its hallway healthcare crisis.
Brampton only has one full-service hospital, Brampton Civic, with an emergency room, which operated between 101 percent and 106 percent capacity in 2019, according to data obtained through a freedom of information request by the provincial NDP last year. The recommended standard of care states hospitals should not operate at more than 85 percent capacity. In the beginning of 2019, Peel Memorial operated at 557 percent capacity, a number that increased to 587 percent from April to June.
In Mississauga, while hallway healthcare is not as big of an issue, wait times to be admitted to the emergency room are long. In its 2019-2024 roadmap, Trillium Health Partners (THP), which operates Credit Valley, Queensway and Mississauga Hospital, described its current setup as “under-resourced for the size and needs of the community.” THP added that no hospital network in Ontario will receive more demand for acute services across the next two decades.
At Mississauga Hospital, the average wait time is 21.2 hours, longer than Brampton Civic, ranking it 100 out of 113 hospitals included in the data. Only eight of the hospitals included have worse averages than 105th placed Credit Valley Hospital, where patients wait for an average of 23.7 hours to be admitted.
The dire situations described in Brampton and Mississauga’s hospitals before the COVID-19 outbreak raise the question of how they can possibly handle worsening rates of infection and the increase of patients and decrease in medical supplies that come with them.
In Ontario, COVID-19 infections are on the rise, resulting in the widespread fear that essential supplies keeping frontline healthcare workers safe will run out. Supplies of N95 respirator masks, which remove 95 percent of airborne particles breathed through them, can become depleted fast. On March 24, the province secured one million N95 masks, six million surgical masks and 12 million sets of surgical gloves. But it’s not clear when further supplies of protective equipment will arrive and when hospitals and other medical facilities will get the needed supplies.
On March 17, Premier Doug Ford announced $100 million in funding for increased capacity at hospitals to provide treatment to people infected with COVID-19, both in critical care and medical beds. Despite the announcement, there is no information on how funds will be distributed and if all medical facilities will get an equal amount of money.
While COVID-19 infection updates from the regional and provincial governments give some localized information to help the public understand how the disease is spreading in a given municipality, it's nearly impossible to identify the spread at a hyper-local level.
One thing that could stop the spread of COVID-19 is a complete lockdown of the country, something Prime Minister Justin Trudeau has not committed to at this point. At the provincial level, while all non-essential businesses are closed, a lockdown hasn’t happened in Ontario. In Peel, the tone is different, with Regional Councillor Michael Palleschi wanting the option of a lockdown on the table.

Prime Minister Justin Trudeau hasn't committed to a full-scale lockdown, something that could drastically impact the spread of COVID-19 in Canada but continues to encourage social distancing and isolation
“If we don't complexly lock down this country, we’re not going to be out of it in five months, eight months, 12 months. I don't know what sort of advocating that needs to be taking place but I think that's a discussion we need to have now,” Palleschi said during a special council meeting Wednesday. The matter will be raised at the regional meeting on Thursday.
According to a 2009 study conducted by the World Health Organization, communication is critical during any pandemic. “Proactive communication...allows the public to adopt protective behaviours, facilitates heightened disease surveillance, reduces confusion and allows for a better use of resources, all of which are necessary for an effective response,” the study reads.
Another confusing discrepancy in information came from the Ontario Ministry of Health, which repeatedly reports fewer or more confirmed cases of COVID-19 than Peel Public Health. For example, in its 10 a.m. update on March 24, the Ontario Ministry of Health confirmed three new cases of COVID-19 in Peel. However, Peel Public Health confirmed 13 new cases on the same day, which may represent a lack of communication between the region and province, causing numbers to lag behind. The Pointer inquired with the regional and provincial health agencies as to where the difference in reported cases originates from.
The Ontario Ministry of Health told The Pointer the cases reported online by the province are based on information from the Public Health Ontario Laboratory and hospitals analyzing COVID-19 tests. “While we make every effort to coordinate and validate with local public health units, there may in some cases be a lag in information sharing at time of posting,” the ministry stated in an email. The Pointer asked if the government would include this information on their website but the question was left unanswered. After multiple inquiries from The Pointer on how many ventilators the provincial government has available to send to hospitals, the Ontario Ministry of Health stated it has more than 1,300. Information on when and how these ventilators will reach hospitals was not provided. Ventilators are crucial equipment needed for treating serious cases of COVID-19.
The Ontario Ministry of Health has stated that it will begin to triage COVID-19 testing. “Health care workers, those admitted to hospital with acute respiratory illness, those with acute respiratory illness who live in long term care homes and retirement homes, and First Nations community members living on-reserve with acute respiratory illness are being prioritized for testing,” the Ministry stated in an email. “The laboratory recently updated its test turn-around times from a 24-hour turn-around time to up to 4-days for the turn-around of test results.”
Meanwhile, Brampton Mayor Patrick Brown said he wants full transparency for the residents of his city. “I think we’re being honest with people that it’s not going to be a matter of weeks but months. I’m not interested in any point in misleading the public,” Brown said during the Wednesday meeting. Regional Councillor Martin Medeiros asked for more specific information on the deferral of property taxes for residents. “[There] has to be that clarification that this is not the waiving for five months but the deferral of five months,” Medeiros said.
The Pointer also raised multiple questions to Peel Public Health, including why the organization didn’t include information about where a patient tested positive for COVID-19. None of the questions were answered in time of publication.
Email: [email protected]
Twitter: @nida_zafar
Tel: 416-890-7643
Submit a correction about this story


