
“It’s probably going to get worse before it gets better”: Peel sees 520% increase in opioid emergencies
Since the insidiously addictive qualities of opioids began to capture national attention more than a decade ago, Peel Region has been spared some of the epidemic’s more devastating impacts.
That could soon change, as recent data shows the region is seeing a spike in deaths, hospitalizations and emergency department visits connected to opioids since such statistics began to be recorded in 2016.
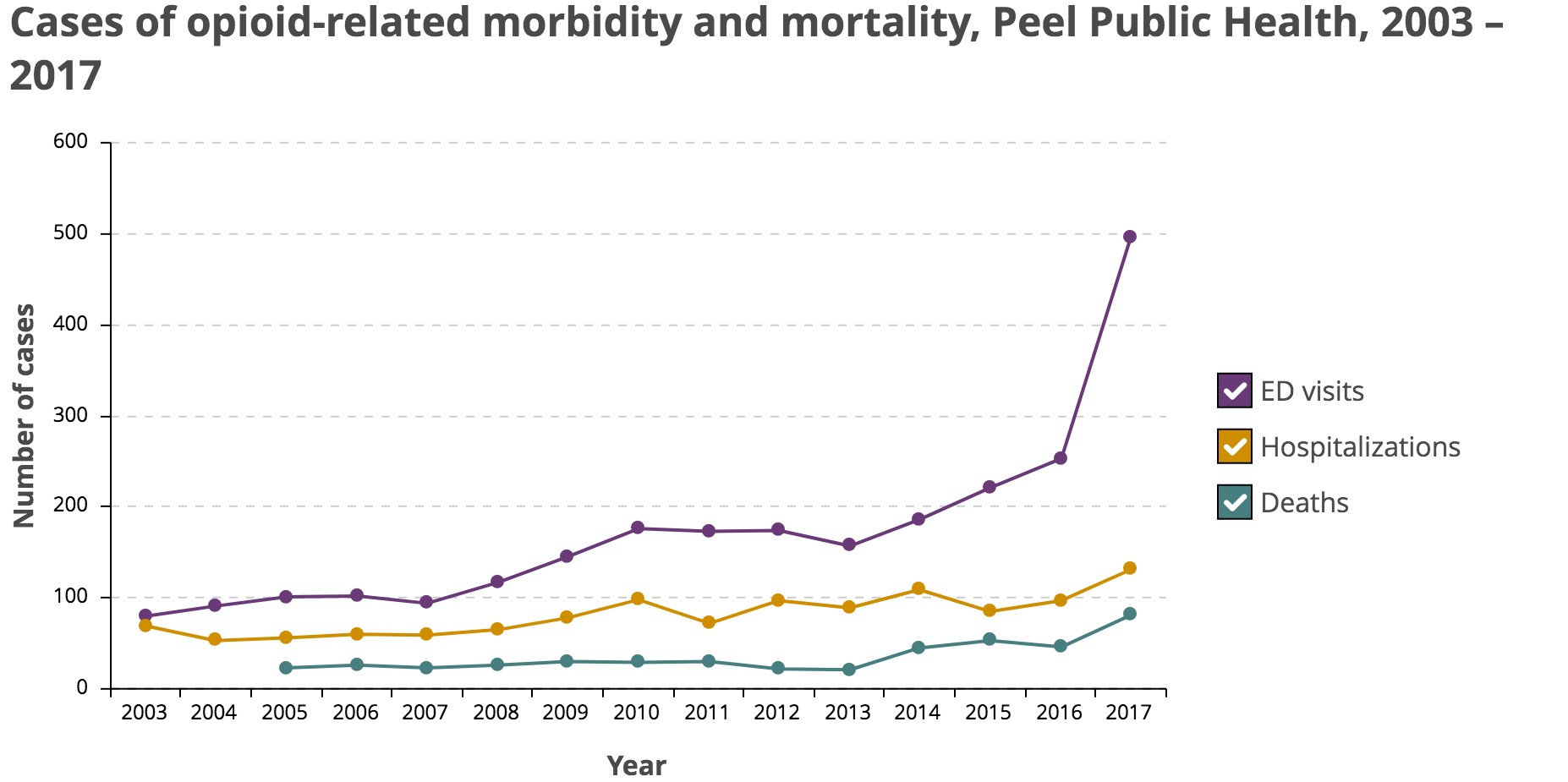
According to data from Peel Public Health, the region saw 496 ED visits related to opioids in 2017 (the latest year for which complete data is available). This is not only an unsettling 96 percent increase over the 253 ED visits in 2016, but a shocking 520 percent increase from 2003 numbers. Through nine months of 2018, Peel experienced 254 ED visits related to opioids.
Hospitalizations and deaths also increased dramatically. The number of people admitted to hospital for opioid use increased 35 percent between 2016 and 2017 (an 89 percent increase from 2003), and the number of deaths from opioid overdose increased from 23 in 2005 to 81 in 2017, a 252 percent increase.
Peel is not an outlier, as similar trends are being observed across Ontario and the country. By comparison, Peel’s numbers are actually quite low. Hamilton, Durham, Ottawa, Toronto and Halton Region all see higher ED visits per capita related to opioids. However, signs are emerging that Peel should be paying attention to.
“Our rates are certainly very concerning; we’re following the same trends in Ontario in our deaths and our non-fatal overdoses, and we’re seeing the very same uptick since 2015/16,” says Dr. Kate Bingham, the associate medical officer of health for the region and the senior lead on Peel’s opioid strategy. “It’s probably going to get worse before it gets better.”
The roots of the opioid epidemic stretch back more than 20 years, wrapped around a now mostly defunct painkiller called Oxycontin.
The drug was widely marketed in 1996 by pharmaceutical giant Perdue Pharma as a non-addictive form of pain management.
Now, two decades later, a United States Justice Department investigation has found the company knew almost immediately their miracle drug was being crushed and snorted illicitly and that it was in fact extremely addictive, but decided to keep quiet. Now, Perdue is being sued by a number of U.S. states for its role in pushing the addictive drug. Most recently, the province of Ontario joined a proposed class-action lawsuit launched by British Columbia in a bid to hold a number of opioid manufacturers accountable for their role in the opioid epidemic, including Perdue.
While that fight goes on in the courts, another, more deadly fight is playing out on streets across North America, one that has claimed the lives of more than 11,500 Canadians since 2016. According to numbers from the National Institute on Drug Abuse, 130 people die every day in the United States after overdosing on opioids.
In Canada, the beginnings of the opioid crisis began in the west, with Vancouver being hit particularly hard by the powerful drug, as well as the more recent emergence of other, more powerful synthetic opioids like fentanyl and carfentanil, which have found their way into the street drug supply. The state of things caused the B.C. provincial health officer to declare a public health emergency in response to the number of overdose deaths in 2016.
“The recent surge in overdoses is a huge concern for us,” said Health Minister Terry Lake at the time. “We have to do what’s needed to prevent overdoses and deaths, and what’s needed is real-time information. Medical health officers need immediate access to what’s happening and where, so they can deploy the necessary strategies to prevent these tragedies.”
The move served as a cue for Peel Region.
“We were starting to see the early signs of a similar situation evolving in Ontario,” says Bingham. “Our community partners were starting to tell us that the picture was changing.”

Dr. Kate Bingham, the associate medical officer of health for the region and the senior lead on Peel’s opioid strategy.
Following B.C.’s decision, the Peel public health unit began to take concrete steps toward defining its role in battling the effects of opioids in the region. This mostly meant a focus on harm reduction, promoting distribution of the overdose-reversing life-saver naloxone through local pharmacies, as well as monitoring overdose and drug-related incidents in the region. The latter was difficult because of a lack of available data. Public Health Ontario had yet to launch its Opioid Dashboard, which now makes opioid-related data on ED visits, hospitalizations and deaths across the province readily available.
“The timeliness of data availability has gotten a lot better in the last two years for a variety of reasons, one of which has been a real focus on specifically getting the opioid data moving more quickly,” Bingham explains.
The importance of up-to-date information cannot be underestimated, as the information allows the public sector to make informed, evidence-based decisions, which translates to an effective use of taxpayer dollars. However, when it comes to drug use, getting a full picture through data alone is difficult.
Most of the data available is related to the harm side of the equation (ED visits, hospitalizations, deaths, etc.), and very little is available to paint a full picture of those using drugs in the region. Prescription data shows the number of pills that have crossed pharmaceutical counters, but does little to capture illicit drug use. Illegal drug users don’t like to admit their use.
For Peel’s public health unit, 2016 started with mostly a blank slate on the opioid file. It involved building a support system and strategy from the ground up.
“There wasn’t an existing structure to say who are we bringing together and what are we actually going to do about a drug strategy,” Bingham says.
 The first fruit of this labour was a snapshot document of the opioid situation in Peel Region. Released in 2017, “Opioids in Peel: A Profile of Opioid Use and Related Harms” brought together all the known information on opioid use and harms in the region. For the first time, it provided residents with a comprehensive view of the situation.
The first fruit of this labour was a snapshot document of the opioid situation in Peel Region. Released in 2017, “Opioids in Peel: A Profile of Opioid Use and Related Harms” brought together all the known information on opioid use and harms in the region. For the first time, it provided residents with a comprehensive view of the situation.
ED visits, hospitalizations, deaths and illicit use were all on the rise, coupled with high prescription rates. The profile painted a picture of Peel that was pretty common across the province. The region was also observing rising rates of opioid use among its younger populations. According to data from the region, 11 percent of students in Grade 7 to 12 reported having used opioids not prescribed to them in the last 12 months. More than half of these students said a family member was the source of the pills. The commonplace nature of these pills has also already reached the school system, with one in five students believing it was either “fairly easy” or “very easy” to access pain pills without a prescription.
The Opioids in Peel document also showed prescription rates in the region were highest in Brampton.
Bingham acknowledges that the initial document was only the beginning, the first step to “get some work on the ground,” to provide a snapshot of the problem. Now, Peel needed to come up with a solution.
As David Smith describes it, “the whole mental health and addictions system in Peel is fragile.”
The CEO of the Peel Dufferin branch of the Canadian Mental Health Association (CMHA) was directly referring to two things: a growing population, and funding that has not kept up. However, there could be a third factor hovering literally on the peripheries of Peel Region.
First, the entirety of Peel’s healthcare sector is no stranger to a lack of funding.
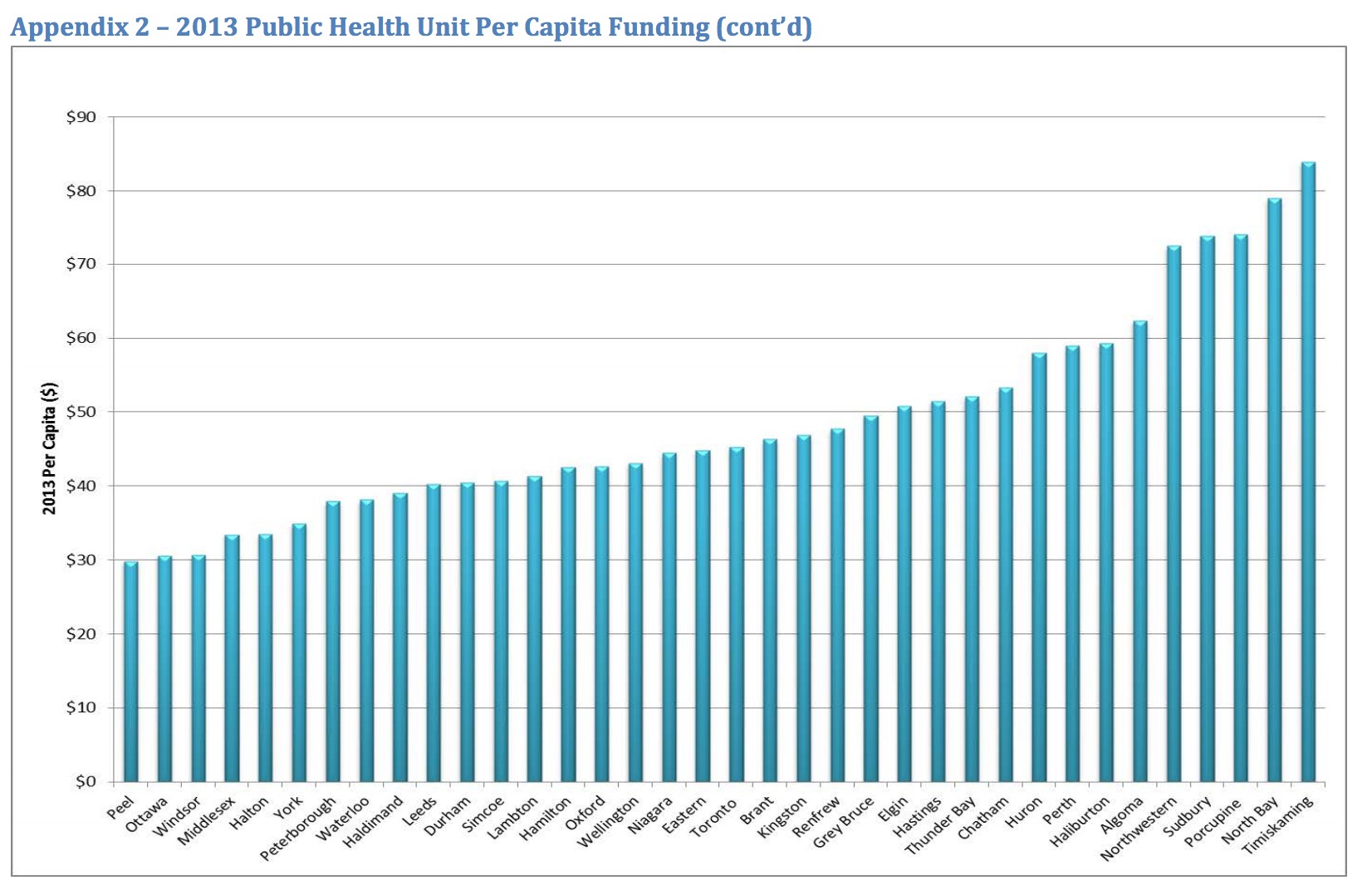
Peel’s public health unit has been chronically underfunded for years. Most of the 35 health units in Ontario rely on the provincial government for about 75 percent of their funding, while local municipalities make up the remaining 25 percent. In Peel Region, however, the Ontario government’s contribution accounts for only 63 percent of the unit’s budget, while the regional municipalities must make up the remaining 37 percent. Now, with recent changes proposed by the Ontario government, the move to a healthcare “super agency” and the amalgamation of the 35 public health units into 10, this funding model will certainly be changing.
And it’s not only public health. Smith’s CMHA branch is one of the lowest funded in the province, and the increasing pressure placed on hospitals by the growing presence of opioids is straining an already stressed system. The Central West Local Health Integration Network (LHIN) has only 0.96 hospital beds per 1,000 people, compared to a provincial average of 2.3 beds.
Considering Bingham’s words that the situation is going to get worse before it gets better, all these factors are even more significant.
Peel’s two LHINs (Central West, Mississauga Halton), while having some of the lowest ED visits and death rates from opioids per capita, are bordered by some of the worst-hit areas in the GTA.
The Central LHIN, which maintains an opioid-related death rate of 5.7 per 100,000 people, is bordered by the Toronto Central LHIN to the south, which has the second highest rate (15.7 per 100,000); the North Simcoe Muskoka LHIN to the north, the third highest deaths due to opioids per capita (15.2) and the second highest ED visits per capita; and the Waterloo Wellington LHIN to the west, the fifth highest in Ontario (13.5 per 100,000).
The Mississauga Halton LHIN is in a similar situation. While also sharing a border with the Toronto Central LHIN, it is bordered by the Hamilton Niagara Haldimand Brant LHIN, which has the fourth highest deaths due to opioids per capita, at 14.5 per 100,000. The Hamilton LHIN also sees the most ED visits per capita due to opioids, at 91.6 per 100,000.

As it stands, Peel remains an island with a death and ED visit rate due to opioids that’s one-third of some of the worst-hit areas of Ontario.
Peel Region staff is continuing to work behind the scenes with the goal of keeping it that way.
Peel’s current efforts to mitigate the impact of opioids in the region is based on a four-pillar strategy informed by the work previously completed for the Opioids in Peel document.
This “four pillar” approach is a standard used across Ontario to develop a holistic approach to dealing with substance abuse. It involves:
1. Prevention: stopping harmful drug use before it happens, for example by changing prescription practices and carrying out education campaigns around the risks of opioid use.
2. Harm reduction: tools that help reduce the impact on those using drugs, such as supervised injection sites and naloxone kit distribution.
3. Treatment: programs and services that assist those looking to stop using harmful drugs. These include improved access to medically assisted treatments such as methadone, and better access to treatments generally, especially for First Nations communities.
4. Enforcement: The pillar handled by the police involves halting or at least disrupting illicit drug sales and distribution.
Bingham explains that no one of these pillars is more important than others, but all of them work together to support the overall opioid strategy and are very much linked when it comes to solving the problems that come with illicit drug use.
“We want to keep people alive, but we also want to prevent people from getting into a situation in the first place where they’re worried about not surviving,” she says. “We’re never going to get ahead of keeping people alive if we don’t also work on trying to keep people healthy in the most holistic sense of the word.”
In Peel Region, approximately 30 groups take part in some level of the strategy, whether through treatment services, handing out harm-reduction supplies, or providing needed therapies.
Under its mandate to promote a healthy lifestyle for residents, it makes sense for Peel Public Health to lead the harm reduction and prevention pillars, but the department also helps keep the entire system on track.
“We’ve been providing a sort of secretariat support to all four, and been holding the surveillance data pieces as well as urgent response planning and policy coordination,” Bingham says.
The region also operates a mobile needle exchange program which, thanks to a funding boost from the previous Liberal government, expanded to two teams in recent years. The vans travel around the region Monday to Saturday, operating on an on-call basis, handing out naloxone, safe inhalation kits and other harm reduction supplies. The service continues to see rising call volumes.
For residents across the GTA, the most visible, and most controversial, aspect of any opioid strategy is the presence of supervised injection sites. Peel Public Health is studying the potential and need for such a site in Peel Region.
The Peel HIV/AIDS Network (PHAN) was approved for an overdose prevention site in 2018. However, the organization, which has since changed its name to Moyo Health and Community Services, lost its funding for the site following the June election and the new PC government’s decision to change the rules for allowing such sites.
“I would say that’s unfortunate,” Bingham says. “We were certainly as supportive in terms of providing the harm-reduction services that we would be to any of our community partners.”
Peel’s ongoing study is aimed at identifying whether such a facility is needed in Peel, the models used in other areas, and what barriers to these sites might be. The study involves online consultation, a survey of drug users and discussions with representatives of other interested groups.
“We’re expecting to have some results to share later this year, hopefully by the end of the spring,” Bingham says.
As is stands, the health sector in Ontario remains fraught with uncertainty. The amalgamation of provincial service agencies and LHINs and funding uncertainties have created many question marks for those fighting the opioid crisis across the province.
Meanwhile, Peel continues to work on expanding its current opioid strategy into a full-fledged drug strategy for the region. Such a strategy would address all substance abuse issues and drugs, as opposed to solely taking on the opioid issue.
“What’s difficult is the complexity and all the factors that contribute to harmful substance use, and getting ahead of the problem really requires going upstream into the prevention” side of things, Bingham says. “That takes time to do, so while we’re trying to figure out what is most effective there, … we need to also work on the downstream pieces, to actually try to keep people alive long enough to improve their health, improve their stability, whatever their goals are in terms of where they’re at and their substance use.”
While things may be changing at Queen’s Park and uncertainty prevails, Bingham knows one thing won’t change.
“The need remains, the work remains, and I think regardless of what the end structure actually looks like, we’re going to be working to make that transition as seamlessly as possible in order to keep up the momentum on the work that we’ve started as the pieces shift around us.”
Email: [email protected]
Twitter: @JoeljWittnebel
Submit a correction about this story


